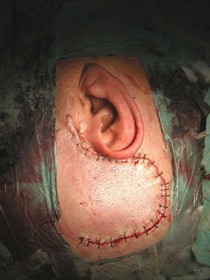
BASE CRANICA è il termine usato per descrivere l’area del cranio che rappresenta la base sulla quale poggia il cervello, comprese le orbite, i condotti uditivi, le arterie carotidi e vertebrali, i 12 nervi cranici ed il sistema venoso di drenaggio del cervello. Ogni nervo del corpo che porta segnali da ed al cervello passa attraverso di essa. La presenza di queste strutture rendono la base cranica una delle aree più complesse da operare. Tradizionalmente molti tumori del basicranio erano considerati inoperabili, perchè con le tecniche chirurgiche ed i mezzi del passato sui pazienti incombeva un grosso rischio di deficit neurologici e mortalità elevata. I progressi della diagnostica per immagini, delle tecniche chirurgiche e dello strumentario (microscopi operatori, monitoraggio elettrofisiologico dei nervi cranici…) hanno permesso ai chirurghi la rimozione di questi tumori con bassa morbidità.
Il concetto base della chirurgia del basicranio è quello di approcciare il tumore rimuovendo una specifica area di osso del cranio per permettere l’esposizione del tumore evitando la retrazione cerebrale. Proprio per questo a volte è necessario passare attraverso l’osso temporale, attraverso l’orbita, attraverso il volto, etc. Massimizzare l’esposizione del tumore per effettuare la rimozione dello stesso preservando quanto più possibile le funzioni neurologiche.
SCHWANNOMI- 10% di tutti i tumori primitivi.
MENINGIOMI- 22% dei tumori primitivi intracranici.
Fossa cranica anteriore- Angiofibromi, estesioneuroblastomi, papillomi invertiti,ca. nasoetmoidali, cordomi, etc..
Fossa cranica posteriore- Neurinomi e meningiomi dell’APC, meningiomi petroclivali, epidermoidi, granulomi colesterinici, displasia fibrosa, ca. del temporale.
Tumori vascolari che invadono la fossa posteriore: TUMORI GLOMICI.<< Nuovo campo del testo >>
APPROCCIO PER FOSSA CRANICA MEDIA: Colesteatoma della rocca
Skull-base Surgery
Lesions of the skull base present a unique challenge to neurosurgeons. In fact, there are very few neurosurgeons in the world who are specially trained and highly qualified to perform such intricate surgery in the small recesses of the brain. Dr. Maroon is part of this minority of experienced surgeons. Our neurosurgeon at UPMC also staff have experience in cerebrovascular surgery and perform vascular skull base surgeries. These may involved management of complex vascular and neoplastic (cancer) lesions of the skull base.
UPMC Presbyterian University Hospital maintains a 24-hour emergency service for stroke, as well as emergency aeromedical transportation.
As a patient, the following information should help you understand the skull base and what is involved in skull base surgery. Skull-base surgery can be performed in several ways, depending on the location and type of tumor or vascular lesion. The information listed below is not intended to take the place of a physician’s explanation, but designed to answer some common questions and make you familiar with terms and procedures related to skull-base surgery.
Skull base is the term used to describe the area of the skull that provides the base on which the brain rests. Contained within the skull base are the eye orbits, ear canals, two carotid arteries, two vertebral arteries, 12 cranial nerves and the blood drainage system of the brain. These many intricate structures make the skull base one of the most complex areas on which to operate.
What are the cranial nerves and why are they so important?
There are 12 pairs of cranial nerves. Each pair of nerves is responsible for a specific, basic function such as blinking, swallowing or focusing the eyes. One of each pair of cranial nerves provides feeling and function, or innervates, the right side of the body and the other nerve in the pair innervates the left. Many tumors of the skull base can affect the cranial nerves, both by their presence and by the steps the surgeon must take to remove the tumor. The result may be a permanent or temporary loss of function of one or more of the cranial nerves. Your surgeon will be able to discuss your specific situation with you as well as your risk of damage to the cranial nerves.
First Cranial Nerve (olfactory nerve) – This nerve is responsible for smell. If injured by tumor or surgery for tumor removal food taste is also altered.
Second Cranial Nerve (optic nerve) - This nerve is responsible for vision. A partial injury to this nerve may result is a “field cut” or partial vision loss.
Third, forth, and sixth Cranial Nerves (oculomotor, trochlear, and abducens) - These nerves are used to control movement of the eyeball. Injury can cause double vision. The third also controls pupil dilation.
Fifth Cranial Nerve (trigeminal nerve) - This nerve controls both function and sensation of the face and if damaged can result in difficulty chewing and diminished facial sensation or facial numbness.
Seventh Cranial Nerve (facial nerve) - This nerve controls facial movements. An injury can result in a facial “droop”.
Eight Cranial Nerve (auditory or acoustic nerve) - This nerve is responsible for hearing. Skull-base surgery can sometimes leave hearing intact once a tumor on this nerve is removed.
Ninth Cranial Nerve (glossopharyngeal) - This nerve is responsible for sensation to the back of throat.
Tenth Cranial Nerve (vagus nerve) - This nerve protects against choking, and allows for normal swallowing and speech.
Eleventh Cranial Nerve (spinal accessory nerve) - This nerve responsible for shrugging shoulders.
Twelfth Cranial Nerve (hypoglossal nerve) - This nerve is responsible for tongue movement.
Two kinds of disorders may make skull-base surgery necessary for your patient. The first, vascular lesions, include aneurysms, malformations of the veins and arteries, and fistulas. The second are benign and malignant tumors. As you are aware, benign tumors also may be life-threatening; we will work with you to determine whether surgical intervention is necessary.
Recent advances in skull-base surgery
Traditionally, many tumors at the base of the skull have been inoperable. In the past, surgical techniques simply were not satisfactory, and many patients faced a high risk of neurological problems after surgery.
Advances in diagnostic imaging, surgical techniques and instruments, and a better understanding of the skull-base anatomy have allowed neurosurgeons to remove tumors at the base of the skull. Previously inoperable lesions now may be removed with far fewer risks to the patient.
Identifying such lesions has become less difficult during the past few years thanks to the advent of magnetic resonance imaging and angiography, among other diagnostic tools. Early detection allows the surgeon to operate sooner and may prevent many complications. Because most tumors of the skull base are benign, early treatment is crucial to prevent a malignancy and maintain optimal function of nerves and arteries in this area.
Reaching the recesses of the brain
Skull-base surgery involves operating within one of three regions of the skull: the anterior, middle or posterior fossa. Neurosurgeons who work within these areas must approach each in a very specific way with regard to the size and type of lesion to be removed. Because of the delicate nature of this type of surgery, patients may be in the operating suite from six to as many as 15 hours or more.
Meningiomas are the most common types of tumors found in this region of the skull base. This benign tumor commonly extends through the skull-base bone and down into the bones of the face. Other types of tumors commonly found in the anterior fossa are pituitary and olfactory lesions, and aneurysms.
To reach such tumors, the neurosurgeon may be required to gently retract the brain from the skull base, allowing removal of the tumor and nearby bone. On occasion, surgeons must use transorbital, transfrontal or transsphenoidal routes to expose and remove the tumor mass.
The middle fossa(blue section on drawing)
The middle fossa of the brain may be approached transtemporally, subtemporally, transfrontally, pterionally or transsphenoidally. The surgical team at ANI’s Center for Skull-base Surgery often will include both a neurosurgeon and otolaryngologist to operate within the complicated anatomy of this region of the skull base.
The posterior fossa(gray section on drawing)
Neurosurgeons often reach lesions in this area of the skull base through the mastoid region and/or labyrinth of the ear. As such, the base of the skull and posterior fossa are clearly exposed to aid in removing lesions within this area. The posterior fossa also may be approached transorally – by way of the roof of the mouth – to gain access to the skull base.
Located in the midportion of the brain, the cavernous sinus houses the carotid artery and multiple cranial nerves. In this small but extremely complex region, it was once virtually impossible to remove lesions. Largely in part due to advanced surgical techniques, extensive experience, specific anatomic knowledge and specialized instrumentation, successful surgery within the cavernous sinus now is possible. The neurosurgeons at ANI’s Center for Skull-base Surgery collectively have a large pool of experience with surgical treatment of cavernous sinus pathologies.
Certainly one of the key aspects of skull-base surgery is reconstructing the skull base after a tumor has been successfully removed or aneurysm has been clipped. Again, it is imperative that the breadth of expertise is vast among surgeons performing these delicate procedures; there must be no chance that the brain will herniate into the nose or surgical cavities or the cerebrospinal fluid does not leak. Often, reconstruction may require taking tissue from another part of the body to create planes and form a successful sealant. Bone from other parts of the skull also may be used in reconstruction procedures.
Disclaimer:
Every effort has been made by the author (s) to provide accurate, up-to-date information. However, the medical knowledge base is dynamic and errors can occur. By using the information contained herein, the viewer willingly assumes all risks in connection with such use. Neither the author nor UPMC shall be held responsible for errors, omissions in information herein nor liable for any special, consequential, or exemplary damages resulting, in whole or in part, from any viewer(s)’ use of or reliance upon, this material.
CLINICAL DISCLAIMER:
Clinical information is provided for educational purposes and not as a medical or professional service. Person(s) who are not medical professionals should have clinical information reviewed and interpreted or applied only by the appropriate health professional(s).
For questions or comments, please contact: bostj@upmc.edu
© 2008 Tri-State Neurosurgical Associates – UPMC
Last Updated: January 1, 2008